

What is rhinosinusitis and how do we get it?
Rhinosinusitis is an inflammation of the lining of the nasal passages and paranasal sinuses. It is not always believed associated with or caused by bacteria. There are several forms of rhinosinusitis. These include: acute, subacute, chronic, recurrent acute and acute exacerbation of chronic. Chronic rhinosinusitis may be seen with or without nasal polyposis.
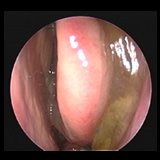
Nasal Polyp blocking air flow
Nasal Polyps are benign tumors of the upper airway which are often time associated with many eosinophils (a type of white blood cell). They are not believed to have any malignant potential. There are many conditions which are associated with their formation and unfortunately in a given person, it may be impossible to determine what the cause of the polyps is. Most often nasal polyps tend to recur. The speed with which they recur is often associated with failure to comply with ongoing medical therapy. Steroids are often very effective in reducing their size temporarily. Rarely aggressive sinus tumors or malignancy can appear within polyps.
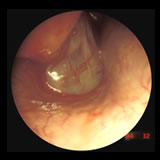
Polypoid change of Left middle turbinate with eosinophilic mucin
Swelling around the small openings to the sinuses caused by environmental irritants, viruses, allergy, or other conditions can result in rhinosinusitis. The mucus in the nose and sinuses can secondarily become infected by bacteria or fungi. It is suggested that forceful nose blowing can lead to contamination of the sinuses with organisms and therefore is best minimized. When the blockage occurs, swelling of the sinus lining can disable the cilia and the drainage of the mucus blanket.
Most episodes of rhinosinusitis are believed initiated with viral upper respiratory tract infections (eg the common cold or flu) (see information sheet on Is it a Cold or Rhinosinusitis?). Those with a genetic predisposition towards allergy, immune dysfunction, aspirin sensitivity, and chronic rhinosinusitis seem to be most susceptible to the long term effect of viral infections or .
Environmental pollutants in the air, such as cigarette smoke, can cause increased irritation of the nasal and sinus passages, particularly in people with hypersensitive nasal lining (mucosa). We are also becoming more aware of the effects of both general outdoor and indoor pollution. Chemicals used in the manufacturing of carpets, furniture, or buildings may also be a problem for sensitive individuals.
If you have allergies, your nose may react to allergy-inducing substances in the air, such as dust or mold. Allergic nasal and sinus swelling may in turn lead to sinusitis. Food allergies (or sensitivities) can also be an unrecognized cause of nasal congestion and swelling. Lastly, certain conditions that exist within your own body can increase your susceptibility to sinus infections. For example, periods of emotional stress can result in swelling of the nasal lining. Certain medications used to treat high blood pressure can also do this. Or, if you have diabetes, high blood sugar can make you more prone to infections in general. Be sure to inform your physician if you have, or suspect, any medical problems.
It is possible that Gastroesophageal Reflux Disease (GERD) may cause symptoms of rhinosinusitis, including chronic cough and post-nasal drainage, but this hypothesis is not fully proven. This may be due to irritation caused by excess acid from your stomach splashing up into your throat. If you have symptoms resembling GERD, such as frequent acid indigestion/heartburn or a tightness sensation in your throat upon swallowing, you will be given further information and instructions.
Ongoing Research to Improve our Understanding of Chronic Rhinosinusitis
A variety of centers throughout the world are engaged in laboratory and clinical research to better improve our understanding of this disorder. There is growing evidence to suggest certain bacteria and or molds may play a substantial role in sustaining chronic rhinosinusitis. Currently, these ideas are getting a lot of attention but they are not yet proven. The organisms attracting the most attention are bacteria called Staphylococcus aureus and Pseudomonas aeruginosa and fungi called Alterneria and Candida (molds and yeast). The three leading ideas describing possible reasons for chronic rhinosinusitis are referred to as the :
Super-antigen Hypothesis
It has been demonstrated that certain toxins produced by Staph. called “super-antigens” can stimulate and “short circuit” our immune response. Other organisms are known to produce toxins but whether or not they can stimulate the immune system the same way is not well studied. The end result is that certain white blood cells called eosinophils are produced in abnormal quantities and sent from the bone marrow to the sinuses where they release toxic substances. Eosinophils sustain the inflammation seen in chronic rhinosinusitis with or without polyps.
Fungus Induced Rhinosinusitis Hypothesis
Interestingly, unlike other white blood cells, eosinophils seem to have a primary function of killing macro organisms such as worms and fungi. Thus, fungi also attract eosinophils and appear to play an important role in chronic rhinosinusitis. Non-invasive fungal rhinosinusitis affects multiple sinuses in young adults. Treatment may include anti-fungal medication, oral steroids, intranasal steroids, oral decongestants, mucolytics and immunotherapy. Functional endoscopic sinus surgery is also a treatment for the management of fungal sinusitis. If there is suspicion of a fungal infection or if your cultures are positive for fungus, you will be treated accordingly.
Biofilm Hypothesis
Staph. species, Pseudomonas and Candida are also known to form protective covering over themselves in a “biofilm” which can tightly adhere to surfaces. Whether or not these are actually present in chronic rhinosinusitis is difficult to prove and laboratory research is currently underway. In this biofilm, under the protection of the “glycocalyx”, these organisms can coexist and share resistance mechanisms to antimicrobial agents. Thus antimicrobials alone have reduced effectiveness when these biofilm are present. This hypothesis ties together the aforementioned ideas and may help explain why some patient improve so much after long course of antibiotics only to relapse shortly after discontinuing the medicines.