

Nasal disorders are traditionally diagnosed through careful history and physical examination. However, sinonasal symptoms can provide limited information for diagnosis. Thus, objective information is sought through physical examination. Although there are many methods available to directly evaluate the nasal passages, three are typically employed for most patients with long standing sinus or nasal complaints. They are: anterior rhinoscopy (looking into the nose with a headlight and nasal speculum to open nostrils), nasal endoscopy (looking into the nasal passages with an endoscope or telescope) and CT scanning. These techniques reveal important information necessary for proper diagnosis, treatment and monitoring. Often times, nasal endoscopic findings compliment findings seen on CT imaging, but they are not always the same. Interestingly, abnormalities detected on endoscopy or imaging can be present without symptoms.
In order to facilitate your nasal examination, your nose will typically be sprayed with a decongestant similar to over-the-counter brands like Afrin® and a topical anesthetic spray, which will numb the lining of your nose. You should inform the nurse at each visit if you are allergic to either of these medications or should you be taking an MAOI (mono-amine oxidase inhibitor) for depression.
When your nose is sprayed please do not sniff in. The spray atomizer will help the medicine be delivered adequately. Sniffing in can lead to more medication being delivered inside your throat than in your nose. Anesthetic spray in the throat can lead cause slight irritation initially followed by a temporary sensation of numbness, perception of difficulty swallowing or even a perception of difficulty breathing even though there is no airway swelling. These side effects can be attributed to the numbness present in your throat. Additionally, you should not drink or eat until you feel normal return of sensation of your throat (about 1 hour) following an examination with these sprays. This is to avoid any inadvertent burn or choking on improperly swallowed food or drink.
The anesthetic spray frequently causes numbness of the front teeth and back of the throat, however, these effects wear off in less than an hour. Once these sprays have taken sufficient effect, usually after six to ten minutes, an endoscope may be used to exam your nose and sinuses. Either a flexible or rigid endoscope is used. Although nasal endoscopy may be an uncomfortable experience, most patients do not find it to be painful. The endoscopic exam yields useful information regarding the nature and extent of disease present in the nasal cavity and the drainage paths of the paranasal sinuses. The CT Scans give complimentary information but does not replace the value of nasal endoscopy. Please see see below for much greater details regarding endoscopy including photographs)
1. Anterior rhinoscopy
Anterior rhinoscopy is the basic tool of the physical examination that most specifically relates to determining the existence of disease (pathology) in the sino-nasal passages. During anterior rhinoscopy the nostril is spread open with a small bunt speculum and the nasal passages can be directly examined with a headlight. This examination gives limited view of the interior of the nasal cavity.
2. Nasal endoscopy
In contrast to anterior rhinoscopy, endoscopy introduces brilliant illumination into the dark cavities and permits magnified direct visualization of the mucosa, turbinates, and, in post-surgical patients, the sinuses. Nasal endoscopy helps identify redness, swelling, polyps, crusting, mucous, and/or pus deep in the nasal cavity.
There are two types of endoscopes available for evaluating the sinonasal passages—flexible fiberoptic endoscopes and rigid telescopes. They differ mainly in terms of patient tolerance and safety.

Rigid endoscope
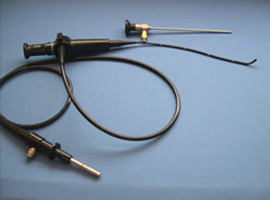
Flexible & Rigid Scope
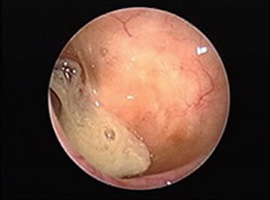
Maxillary Sinus Infection
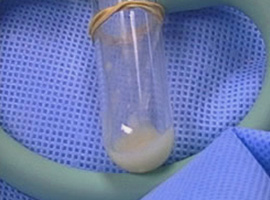
Endoscopically aspirated culture
With regard to patient comfort and direct access to sinus cavities, flexible endoscopy is generally superior to rigid endoscopy. However, image clarity, the ability to obtain cultures and sample tissues, the ability to control epistaxis, and the ability to perform surgery is superior with rigid endoscopy. Photo documentation of an endoscopic evaluation (Photo-Endoscopy) has been used by some as a research tool and to follow patient’s progress. Despite a difference in patient comfort, even rigid nasal endoscopy can be well tolerated. This is evidenced by unpublished data collected during an evaluation of the microbiology of the nasal cavity in twenty healthy medical students. The subjects underwent topical decongestion and anesthesia followed by rigid nasal endoscopy and were asked to rate their overall experience with rigid nasal endoscopy before culture sampling on a 1 to 5 scale. On average, the subjects rated the experience between tolerable and mildly uncomfortable (2.5).
Risks of Nasal Endoscopy
Although it is generally a very safe and very well-tolerated procedure, the most common adverse effects of endoscopy are patient discomfort/pain, nasal bleeding, and feeling faint or lightheaded from anxiety.
Indications for Nasal Endoscopy
These include but are not limited too:
Although some debate exists over the value of endoscopically obtained cultures, many leaders who study nasal and sinus diseases collect them to guide therapy. Cultures should be obtained by skilled experienced endoscopists. Otherwise, the results from the specimen may be misleading. Endoscopic sinus cultures may be performed with either a sterile swab or by suctioning pus into a sterile trap.
3. CT Imaging
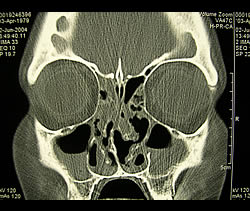
Coronal CT of Sinusitis
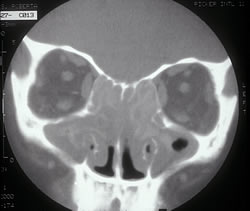
CT of Fungal Sinusitis
This computerized x-ray of the sinuses gives fine detail about soft tissue swelling, the presence of fluid, and anatomic abnormalities deep in the sinus cavities. These images are often best obtained while you lay down on your stomach with your chin down and your neck extended.
Additional tests or studies used to evaluate sinus and nasal problems include but are not limited to: